As we enter 2024, health plans and employers face a complex and challenging scenario shaped by escalating drug costs. The annual increase in drug prices that hit every January is more than a budgetary concern; it’s a critical issue in healthcare affecting the accessibility and well-being of employees and plan members. RazorMetrics has a solution to help self-funded employers and health plans make a dent in pharmacy budgets.
Escalating Medication Prices Sink Budgets
Managing the prescription price spikes is difficult because costs are tied to a multitude of complicated factors like growing demand for specialty drugs, legislative changes, inflationary trends, and greed.
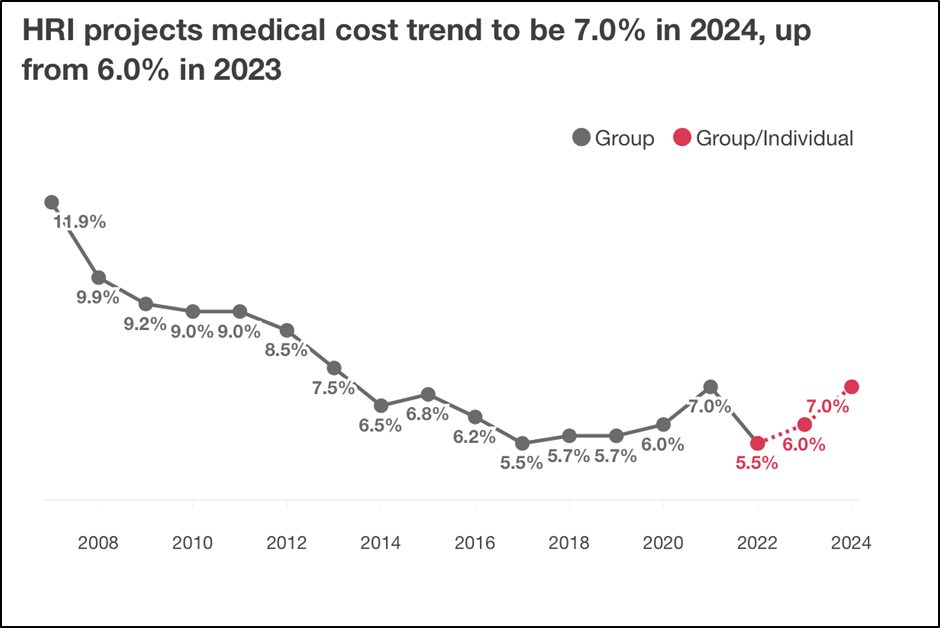
This year, the hit is higher than usual. The recent PwC report projects a 7% increase in healthcare costs, exceeding the hikes seen in prior years. According to experts, the increase is due to a number of factors, including labor shortages, contract negotiations, and the rise of expensive pharmaceuticals, particularly specialty drugs.
Ripple Effects on Health Plans and Employers
The soaring medication prices in 2024 cast a long shadow over health plans and employers. The added financial strain directly impacts healthcare expenses but also influences members’ and employees’ well-being and overall healthcare access.
When healthcare is more expensive, it affects medication adherence. In a blog looking at non-adherence, we examined why adults are not taking medication as prescribed and shockingly, discovered that 13.2% (aged 18-64) reported cost as the culprit. A recent CDC study correlates medication costs with nonadherence, showing that financial barriers lead to patients skipping or reducing doses. The study found that cost-related non-adherence was associated with a 15% to 22% higher mortality rate. High drugs costs are a barrier to treatment and the result is poorer health outcomes and increased hospitalizations that further drive up healthcare costs.
For employers and health plans, these escalating costs present a dual challenge: managing organizational financial health with covered members’ physical health. Additionally, pharmacies are closing across the country due to tumultuous changes in pharmacy retail, hitting underprivileged and rural areas particularly hard. Closures mean patients must find a new way to access their medications, posing further challenges and impacting adherence rates.
Stem the Tide with RazorMetrics
Dealing with these challenges makes solutions like RazorMetrics not just prudent but crucial.
Their SaaS platform is designed to change how doctors prescribe within their regular workflow. It’s all about finding ways to cut costs without cutting corners on care. The Intervention Codex, developed by doctors and pharmacists, dives deep into thousands of medications, analyzing the best fit for a client’s formulary and choosing the most cost-effective options.
With RazorMetrics, health plans and employers have a real shot at managing the impact of rising drug costs while still delivering top-notch healthcare. By providing an innovative, physician-first solution, RazorMetrics is leading the charge in reshaping how pharmacy budgets maximize saving opportunities. It’s not just about crunching numbers; it’s about ensuring tangible, positive outcomes for everyone involved.




